by Kate | Jul 13, 2017
Time: 7am
Location: Labor and Delivery Floor
Attire: Scrubs and Danskos
Occassion: First day on OB/GYN Rotation
“Do you know how to scrub in?” asked the second-year resident, Dr. B, as we speed-walked through endless sets of double doors to the Delivery ORs. “We’ll do it together.”
We stood side-by-side at the huge silver sink basins, already wearing masks and hairnets, and began the ritual of scrubbing. First, we cleaned beneath each of our fingernails with a plastic pick. Then we opened packages of special scrub sponges filled with special soap. When we turned on the water by hitting a huge panel with our hips, a large clock above the faucets turned on, counting down from five minutes. 5:00. 4:59. 4:58. 4.57… Scrubbing is required to take the full five minutes. Scrubbing takes a directed sort of focus, the same feeling I get when I am running; the mind feels at once still and directed, and the rest of the world fades away. I focused on my fingers, imagining each of them as a box with four sides, and proceeded to scrub each side of each finger-box ten times. I did the same to the palm, the back of the hand, the wrist, and the arm all the way up to my elbow, then started on the other hand…
In a hospital world where everything always feels rushed, standing at the sink for a five full minutes, hearing only the water hitting the steel basin, is at once strange and calming. The trickiest part is rinsing: the water must not drip onto any part that you’ve already rinsed. Once you’ve rinsed, NOTHING can touch your skin. As I was finishing up, the clock reaching 0:00, my pinky brushed the string of a mask sitting on the shelf above the sink. I froze. Dr. B chuckled ruefully, “I’ll meet you in there,” she said, heading towards the OR as I reset the clock and began the entire scrubbing procedure again.
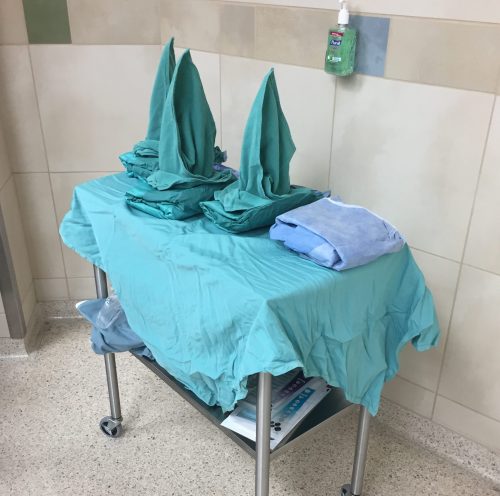
Towels and gowns, out and ready to go!
The second time I scrubbed successfully and backed into the OR, opening the huge doors with my back to protect my newly clean arms. The scrub nurse (in charge of all the logistics in the operating room) handed me a sterile towel, and then held up a sterile green gown for me to plunge my arms into, like a bathrobe going on backwards. The efficiency of the OR staff took me by surprise; the moment my arms entered my gown, a second nurse was at my back, tying the strings. Next, the scrub nurse helped me into my gloves. First the white pair, then the green pair over the top. This way, if the top glove broke, I’d notice the lighter color glove showing through.
I was ready.
The patient was already in the room, lying on the table with her huge belly sticking into the air. Dr. B stood on the patient’s right. The attending physician, Dr. V, stood directly opposite on the patient’s left, directing the show. I stood at Dr. B’s left elbow, my hips resting against the surgical table and my hands on the patient’s leg (protected under a sterile drape). Across from me, the scrub nurse positioned a huge tray of instruments – scissors, scalpels, forceps and towels. Dr. V positioned the huge lights overhead. Anesthesiologists stood by the patient’s head, busy with IVs. The atmosphere was calm, purposeful, and efficient. I stood stock still, afraid to get in the way, unable to diffuse the thought that I was close enough to mess things up badly if I bumped against Dr. B or knocked over the instrument tray.
Everyone’s focus honed in on the square of brightly lit, pregnant belly. With Dr. V’s guidance, Dr. B made the incision and exposed the surface of the uterus. Then Dr. V turned to me. “Kate, put your hand on the uterus and slide it up until you find the top.” I reached, heart beating faster. The dark red uterus was warm and smooth, stretched tight because of the baby inside. I slid my hand up into the abdomen between the skin and uterus, my eyes widening: the uterus was so big! And my hand was inside the body of a LIVING PATIENT! It was a surreal but wonderful feeling.
Dr. B continued the procedure, opening the uterus and breaking the amniotic fluid sac. Dr. V reached inside for the baby. Time stood still as she calmly pulled, spun, and wriggled the baby into the world, exposing a little bottom, two feet, two flexing arms, and finally a tiny face to the air for the first time. The baby scrunched up her face and started to cry, at that moment the most beautiful sound in the world because it meant that she was healthy and safe. As Dr. V carried the baby over to her mother’s arms (free to move behind the surgical drape), she cooed, “Happy birthday, we all love you, welcome, oh happy day! Born at 7:46am on a Monday.”
With a start, I realized that in my first hour on OB/GYN, I had scrubbed into a c-section delivery, touched the inside of a living, breathing woman, and seen a new life come into the world. Hundreds of thousands of babies are born every day – for mother nature birth is routine. But for me it was completely incredible. I scrubbed several more times that day, each time before another c-section, spending the five minutes of calm reflecting on what I was seeing. I might just become an OB/GYN. Oh happy day indeed.

Tired but happy at the end of the day!
Kate is a third-year medical student at University of Michigan Medical School. She is passionate about women’s health, reproductive justice, and finding the humanities in medicine. When not in the hospital, you’ll probably find her running along the Huron River or puzzling over the NYTimes Sunday crossword.
by Kate | Jun 26, 2017
5:15am, my alarm goes off. It’s the beginning of a new day. My M3 clerkships are beginning as well; I’m in the middle of my first rotation: pediatrics.* Today, my inpatient team is on “early call,” which means that we are responsible for taking over care of all the pediatric patients that were admitted overnight. We have to be in at 6am (a half hour earlier than usual) to hear about the patients from the night team. Being early call also means I can wear scrubs rather than dress clothes, so getting dressed is mercifully easy in my half-asleep state. I pack my lunch and head out into the fresh predawn air, walking past newly blooming flowers on my way to the hospital. The promise of beautiful spring day is all around.

Stopping for a selfie with Big Bird on my way in to Mott Children’s Hospital!
At the hospital the night team fills us in, and then it’s time to “preround” on my patients. Using the electronic medical record, I check on their vital signs and fluid balance overnight, read new lab and test results, and jot down my ideas for the coming day’s care plans. After this is done, I visit their rooms, ask how the night was, and perform a physical exam. Ideally, this is all done before 8am, when the medical students and residents have a morning lecture or conference. Even with only two patients, I am almost late. I have no idea how I’ll someday follow eight patients like the interns do!
At 9am, morning lecture is done and it’s time for rounds. Together with the attending physician, senior resident, interns, and sometimes nurses, dietitians, and social workers, we visit each room, talk about the condition of each patient, their plan for the day, and make sure to address any concerns the patient and their family may have. This can take a long time! When our team is full and caring for 22 patients, even if we spend just 10 minutes on each, rounds take almost four hours. I start off the discussion on my patients by reporting what I learned during my early-morning prerounds and stake a stab at their plan for the day (the interns do this for the other patients); the attending physician leads the discussion from there. The more you know about the patients and their conditions, the easier it is to stay engaged during such a long rounds, and I do my best to stay focused.
The afternoon is spent following through on the care plans decided during rounds: we talk to subspecialists (cardiologists, nephrologists, etc.), look at test results, see if new medications are making a patient feel better, and write notes that summarize each patient’s day in their medical record. I try to take a moment when things are calm in the team room to visit my patients again in the afternoon. I find that on my morning rounds I get to know the patients’ medical conditions, and during my afternoon rounds I get to know them a little better as people and families. In the afternoon people are more chatty, and I’m not in such a time crunch. My patients range from newborns to teenagers, in the hospital due to all sorts of things including asthma attacks, pneumonia, kidney infections, feeding difficulties, and constipation. Part of what I like about pediatrics, though, is that children’s bodies are very resilient and most of our patients go home in just a few days!
Soon it’s 4:30 or 5:30pm, and the team is finishing up for the day. The interns stay until 6pm to sign out to the night team, but the medical students usually leave before that as the day’s work is done. I walk home through the late afternoon sun and reflect on the day, happy I’ll have some time to run and cook dinner before studying for a few hours for the shelf (the exam at the end of each rotation). Before I know it, it will be 5:15am, and time to begin another day!
*I wrote this in March…clinical rotations have kept me busy enough that I’m only finishing the post now!
Kate is a third-year medical student at University of Michigan Medical School. She is passionate about women’s health, reproductive justice, and finding the humanities in medicine. When not in the hospital, you’ll probably find her running along the Huron River or puzzling over the NYTimes Sunday crossword.
by Kate | Jan 16, 2017
Happy New Year! It’s 2017, and the M2s are quickly wrapping up with our preclinical curriculum. In six weeks, we will bid goodbye to the lecture halls and anatomy labs for good, don our short white coats, and step into the hospital. I can’t wait! Between now and then, we have a two-week Hematology/Oncology unit (our last unit of new material!), a two-week review period, and a two-week vacation. The vacation is a particularly nice and unexpected gift; it will be wonderful to take a break to relax and fill our sleep reserves before hitting the wards.
Our clinical rotations (these are traditionally done during the M3 year, but we’re getting a head start due to Michigan’s updated curriculum) include blocks spent working with Internal Medicine, Surgery, Pediatrics, Family Medicine, Obstetrics & Gynecology, Neurology, and Psychiatry. We’ll be working in clinic six days a week, though the specific hours will vary depending on which service we are with. I’ve been told I’ll be very busy, but that I’ll also feel more engaged and enjoy clinic more than lectures. Hopefully it works out that way! I start on Pediatrics, and I’m excited to simply dive in and see what working in the hospital and clinics is all about. That, after all, is what I came to medical school to do! Most of my classmates feel the same way: somewhat nervous since there are so many unknowns about working on the wards, but also excited to get started. As much as we’ve learned thus far, I know we’ll learn even more during our clinical time, adding real life experience to what we’ve memorized from our text books and lectures.
Last week we had a short Rheumatology unit, in which we learned about autoimmune conditions affecting the joints. Now that we are reaching the end of our preclinical material, a lot of this unit was review of concepts we’ve seen before. It was nice to see things a second time; while I definitely needed the review, things were a bit easier to remember this time around.

The Botanical Gardens had an exhibit of “botanical clothing.”
I managed to take the test on Friday (we have from Friday afternoon until Sunday night to take our weekly quizzes or exams), which meant I had an entire weekend to enjoy! My free days allowed me to take full advantage of some of Ann Arbor’s many great things to do. On Saturday I went to a movie at the beautiful historic Michigan Theater and had coffee downtown with my parents. Sunday was very cold but beautifully sunny, so I bundled up and went for a run by the Huron River – one of my favorite things to do here whether winter or summer! I spent the afternoon at the UM Matthaei Botanical Gardens, enjoying the warm steamy air and many-colored plants, and finished up the weekend with a game night featuring Settlers of Catan. School keeps me busy, so I always appreciate free time and try to make the most of it.
Stay warm out there!
Kate is a third-year medical student at University of Michigan Medical School. She is passionate about women’s health, reproductive justice, and finding the humanities in medicine. When not in the hospital, you’ll probably find her running along the Huron River or puzzling over the NYTimes Sunday crossword.
by Kate | Oct 6, 2016

In 1893, Anatomy at Michigan was probably taught like this! Now it’s much more hands on, students work in groups of four with each donor.
Anatomy class is an irreplaceable and unique learning experience during our M1 year; a tangible trip through the human body that allows us to explore and learn without fear of causing harm. Without anatomical donors, we would not have this opportunity. I recently spoke at the Anatomical Donations Memorial Ceremony, an event for the families of those who donate their bodies to our education. I thought Dose of Reality readers might enjoy hearing my thoughts as well! Here are the reflections and gratitude that I shared at the memorial:
“To our donor,
Today we learned about the anatomy of the legs. Those words might sound simple, boring maybe, but I want to thank you because with your help, it was amazing. When I got home, I spent a long time in front of the mirror, running my hands over my own legs, finding the structures that I knew were inside. Here is my femoral artery pulsing. I’ll have to live three more lifetimes until it has pulsed for as long as yours did. Here is my Achilles tendon – I never realized just how thick and strong it is until you showed me yours. Here are the soft bellies of each of my muscles, so smooth and so powerful at the same time.
Donor, for the first time I am grasping the beauty that lies beneath the skin, because you selflessly allowed us to see the beauty beneath yours.
I’m not sure if you’re watching, Donor, what we do in anatomy class, so I’m not sure if you know that I was the one who made the first incision that first day of class. I hope you heard me whisper, “thank you,” and heard my classmates later do the same. And if you are listening, I hope you don’t mind when our concentration strays to talking about our classes or to wondering about the future and the types of doctors we will be one day. Then again, maybe you like hearing about the process you stepped into, and knowing about the people you are helping us to become. Rohit said he might become a surgeon! Me, I want work with the same patients over time; so I think I’ll go into primary care. You’ll probably laugh when we all end up somewhere different than where you heard us plan this semester. Like a good advisor, you’ve helped foster our dreams, confident that whatever we do will be worthy of your help. We won’t let you down.
I wonder about what you did, in your life. You graciously share with us some of the most personal elements of you, but other things are left unsaid. These hands, did they once cradle new life? Your well-worn feet, to what corners of the world did they walk? I held your heart; did it beat strong and nervous in love? You can’t tell us, but just know that we wondered, and appreciated that the answers are important, even if we can’t know.
It is incredible to think, Donor, that you started as one tiny cell. That the one cell multiplied and changed and grew and formed all of you – all the structures we learn from and marvel at, all the things we can’t know. I think about that amazing fact almost every class. At the end of the day, we learn the anatomy and physiology, but I think the most important thing you teach us is just how beautiful and incredible this thing we call life really is, and for that I thank you.”
Kate is a third-year medical student at University of Michigan Medical School. She is passionate about women’s health, reproductive justice, and finding the humanities in medicine. When not in the hospital, you’ll probably find her running along the Huron River or puzzling over the NYTimes Sunday crossword.
by Kate | Aug 18, 2016

Med students and residents with Dr. Howell at the concert.
This story starts back in February, in Rackham Auditorium at a piano concert. UM’s University Musical Society was presenting Sir Andras Schiff, with his program, “The Last Sonatas,” in which he played the last three sonatas written by Mozart, Beethoven, Haydn, and Shubert over a series of three concerts. Waiting for the performance to begin, a few classmates and I were chatting about our interest in music, and one announced that he was planning a small concert of performances by medical students, and we should all consider taking part. Music! A night full of music, for an audience of friends! I’ve long been involved in music, first with private lessons and then through school-based ensembles, but after graduating college it had been harder to find chances to play and sing. How could I resist? I agreed to perform. Voice has been my instrument of choice in recent years, but I decided on the spot I would play the piano. The unassuming Sir Schiff walked across the stage, sat down at the piano, and began to play Beethoven’s “Piano Sonata No.30 in E major, op.109.” A smile grew on my face as the notes danced around us. I tapped my fingers on the arms of my chair; soon they would be playing on keys. (more…)
Kate is a third-year medical student at University of Michigan Medical School. She is passionate about women’s health, reproductive justice, and finding the humanities in medicine. When not in the hospital, you’ll probably find her running along the Huron River or puzzling over the NYTimes Sunday crossword.






